ADHD Treatments & Therapies
The Australian National Clinical Guidelines for ADHD recommends medication as as primary treatment for ADHD, and do not recommend Neurofeedback. However, the guidelines states that "Combined pharmacological and non-pharmacological treatment was better than either alone. Each mode was more effective than the other in targeting specific aspects of ADHD: Pharmacological treatments were more effective for reducing core ADHD symptoms, and non-pharmacological treatments were more effective for improving functional outcomes for people with ADHD. The following are the options for ADHD treatments:
- Stimulant or non-stimulant medication
- Counselling
- Cognitive Behavioural Therapy
- Family Therapy
- Neurotherapy
- Diet & Nutrition
We will discuss the above methods in detail below.
Medication for ADHD (from a medical professional)
For decades, stimulant medications have been used to treat the symptoms of ADHD. While stimulant medications remains the most recommended first line medical treatment, Approximately 40 to 50% of children diagnosed with attention-deficit/hyperactivity disorder (ADHD) either fail to achieve sufficient symptom control or discontinue treatment due to sideeffects or poor tolerability (Faraone, 2009; Cortese et al., 2018; Riera et al., 2017; Lilja et al., 2025). The potential for side effects should be weighed against the benefits before these drugs are prescribed. Children on these medications may lose weight, appetite, and grow more slowly. Others have problems falling asleep.
"""It is under discussion whether stimulant medications aggravate TICS and other Tourette’s symptoms. After noting a child’s height, weight, and overall development, doctors often conclude that the benefits of medication outweigh the potential side effects, and that side effects can be managed by a reduction in dosage. Thus, parents should educate themselves on both sides of the debate before making their decision.
Another question is whether stimulants are prescribed unnecessarily for too many children. Keeping in mind that many things, such as diet, poor nutrition, anxiety, depression, allergies, seizures, and problems at home and/or school make children overactive, impulsive, or inattentive, it is possible the medication is not the full answer. Critics of medication argue that many children without ADHD are medicated to control undesirable behaviours, when dietary changes, nutrient supplements, Neurotherapy and counselling could be tried first.
Unfortunately, for some children, being scolded or punished is the most attention that they get. They have little opportunity to build a sense of worth and competence. Whilst medication can help control behavioural problems that lead to family turmoil, there are often aspects of the problem that medication cannot improve. ADHD is a disorder that has broad emotional and academic repercussions. In the scientific literature there is no evidence that stimulant medication promotes long-term improvements in academic or cognitive areas.
Across multiple meta-analyses, the consensus is that roughly 40-50% of children with ADHD either do not respond adequately to medication or discontinue treatment due to side effects or poor efficacy. This highlights a substantial need for alternative or adjunctive treatments, such as neurofeedback or behavioural therapies. This is in line with the Australian Clinical guidelines for ADHD which states:
"Combined pharmacological and non-pharmacological treatment was better than either alone. Each mode was more effective than the other in targeting specific aspects of ADHD: Pharmacological treatments were more effective for reducing core ADHD symptoms, and non-pharmacological treatments were more effective for improving functional outcomes for people with ADHD.
Treating health professionals should consider combined treatment if it is available, feasible and cost-effective for the person and in the local context, and the available treatment is appropriate for symptoms, function or participation needs."
Counselling for Children with ADHD (by a psychologist)

If children are hyperactive, they are often told that they are naughty and punished for being disruptive. If they are disorganised, and unfocused in tasks, they may be called lazy. If they impulsively grab toys, interrupt conversations, or push their classmates, they lose friends. If they have a related conduct disorder, they may get into trouble at school, or even with the law. People with ADHD often experience the daily frustrations of living with disorder, as well as the fear that others think that they are strange, abnormal, or stupid.
These cycles of frustration, blame, and anger, persist for so long that breaking them is hard. Children and their parents need help to develop healthy techniques for managing these cycles of cognition, affect, and behaviour. A psychologist who counsels the child and/or their family, can help them develop new skills, attitudes, and ways of relating to each other.
In individual counselling sessions, a psychologist helps people with ADHD feel better about themselves. People can learn to recognise that having a disability does not reflect who they are as a person. A psychologist helps people with ADHD identify and build on their strengths, cope with daily problems, control their attention and aggression. In counselling, people learn that they are not alone in their frustrations and that help is available.
Sometimes only the person with ADHD requires counselling. Yet in many cases, all family members need support due to the functional impact of ADHD. A psychologist can help the family find better ways to promote change. If the child is young, most of the psychologist’s work is with the parents, teaching them techniques for coping and improving their child’s behaviour.
Cognitive Behavioural Therapy (CBT) in ADHD
CBT refers to a group of therapies that aim to reduce a person’s dysfunctional cognitions and behaviours by helping them identify and alter their underlying thinking patterns. In other words, you learn to replace maladaptive behaviours with adaptive ones. The basic concept of CBT is that behavioural change has a flow-on effect to other areas of functioning. CBT is a therapeutic intervention which promotes new replacement behaviours, identifies unhelpful thinking patterns, and teaches healthy self-talk. However, there is no evidence that CBT is effective at bringing about permanent change in the core symptoms of ADHD. However, CBT when combined with medication, lifestyle changes, optimum nutrition and/or Neurotherapy, can promote psychosocial skills, minimise low self-esteem, and the ADHD’s biological underpinnings.
ADHD Therapies for Family
Family therapy can help families improve their communication skills. Family therapy involves training in communication, interpersonal relations, conflict resolution skills, boundary setting, and healthy discipline. Not all families require counselling, and those who do may need help only in some areas.
Neurotherapy for ADHD
.jpg)
The Australian National Clinical Guidelines for ADHD recommends medication as as primary treatment for ADHD, and do not recommend Neurofeedback. However, the guidelines states that :Combined pharmacological and non-pharmacological treatment was better than either alone. Each mode was more effective than the other in targeting specific aspects of ADHD: Pharmacological treatments were more effective for reducing core ADHD symptoms, and non-pharmacological treatments were more effective for improving functional outcomes for people with ADHD.Since the early 1970s, research and clinical practice in Neuroscience and Psychophysiology has shown that Neurofeedback (Neurotherapy or EEG Biofeedback) can encourage brain plasticity and promote the normalisation of the brain patterns that underlie ADHD behaviours. In many studies, Neurotherapy has been shown to be as effective as stimulant medication for some children with ADHD.
Neurotherapy is computer-based brain retraining that promotes more normal patterns of electrical activity. It has been shown to be an effective treatment for around 80% of children with ADHD and Learning Difficulties.
In the 1970s, Neurotherapy was developed at the UCLA Medical School EEG Laboratory by Professor Barry Sterman as a therapy for childhood epilepsy. It was further developed by Professor Joel Lubar of Tennessee University as a treatment for ADHD and Learning Difficulties. To date, there are over 300 studies that show Neurotherapy to be an effective treatment for ADHD and learning difficulties. Therapy effects appear to last for years.
Neurotherapy Research Findings
In the January 2000 issue of ‘EEG and Clinical Electroencephalography’, a journal from the EEG and Clinical Neuroscience Society, was a focused review of Neurotherapy. Professor Frank H. Duffy, M.D., a paediatric neurologist at Harvard Medical School, stated that Neurotherapy should play a major therapeutic role. In his opinion ‘If any medication had shown such a wide range of benefits with no adverse side-effects it would be widely used and accepted.’
For a full bibliography of Neurotherapy studies look up:
https://www.dropbox.com/scl/fi/g0x7jjphy599ggzlr0scf/Comprehensive-Neur…
For a synopsis of randomises control trials and meta analyses look up: https://www.dropbox.com/scl/fi/bcqlw192nb3acic8ssu87/Neurofeedback-for-…
Dietary Changes and Nutritional Supplementation from a nutritionist.
‘Diet’ is the term given to what you eat, whilst ‘nutrition’ is what you absorb from your diet.
Optimising Diet and Nutritional Supplements in the Treatment of ADHD: A Review of the Evidence
Attention-Deficit/Hyperactivity Disorder (ADHD) is a neurodevelopmental disorder characterised by inattention, hyperactivity, and impulsivity. While pharmacological interventions are the mainstay of treatment, interest in dietary interventions and nutritional supplementation is growing due to concerns over medication side effects and the desire for holistic approaches. This essay reviews the current evidence from randomised controlled trials (RCTs), meta-analyses, and systematic reviews on optimising diet and the use of supplements in ADHD management.
Dietary Interventions
A number of dietary strategies have been investigated for their potential to reduce ADHD symptoms. One of the most rigorously studied is the "few-foods diet" (FFD), a form of elimination diet that restricts intake to a small number of foods considered unlikely to cause adverse reactions. A meta-analysis by Pelsser et al. (2017) concluded that FFDs can lead to significant reductions in ADHD symptoms in children, with mean effect sizes comparable to those observed with pharmacological treatments (Pelsser et al., 2017). A systematic review by the European ADHD Guidelines Group (2013) also supports the efficacy of FFDs, though practical challenges and the risk of nutritional deficiencies limit their widespread use (Sonuga-Barke et al., 2013).
The impact of specific dietary patterns has also been explored. A systematic review and meta-analysis by Shareghfarid et al. (2020) found that Western dietary patterns (high in processed foods, sugars, and fats) are associated with increased ADHD risk, whereas diets rich in vegetables, fruits, and whole grains may be protective. These observational findings are supported by RCTs indicating that individualised dietary modification can modestly reduce symptom severity (Shareghfarid et al., 2020).
Artificial food colourings and preservatives have long been suspected of exacerbating ADHD symptoms. A meta-analysis of 24 RCTs by Nigg et al. (2012) reported small but statistically significant effects of artificial food colour exclusion on ADHD symptoms, though the effect was more pronounced in children with suspected sensitivities (Nigg et al., 2012).
Nutritional Supplements
Supplementation with specific nutrients has been extensively studied as adjunctive or alternative therapy for ADHD.
-
Omega-3 Fatty Acids: Multiple meta-analyses indicate that omega-3 supplementation, particularly eicosapentaenoic acid (EPA), yields small but statistically significant improvements in ADHD symptoms (Bloch & Qawasmi, 2011; Chang et al., 2018). The effect size is larger in individuals with low baseline omega-3 levels.
-
Minerals: Iron and zinc deficiencies have been linked to ADHD pathophysiology. A meta-analysis by Wang et al. (2017) found that zinc supplementation significantly improved hyperactivity and impulsivity among children with low baseline zinc, while iron supplementation was beneficial in those with ferritin deficiency (Wang et al., 2017).
-
Vitamin D and Magnesium: Recent RCTs suggest that vitamin D and magnesium supplementation may reduce symptom severity, particularly in children with documented deficiencies (Abhishek et al., 2024; Elshorbagy et al., 2018).
Comprehensive Reviews and Recommendations
A 2024 systematic review by Abhishek et al. summarised the evidence for dietary interventions and supplements, concluding that the most robust benefits are seen in children with baseline deficiencies or specific sensitivities. The review also highlighted the need for individualised assessment and the importance of monitoring for potential nutritional imbalances (Abhishek et al., 2024).
A large-scale systematic review by Sonuga-Barke et al. (2013) underscored that, while dietary interventions and supplements can be beneficial, effect sizes are generally smaller than those seen with medication, and interventions should be tailored to the individual patient.
Conclusion
Evidence from meta-analyses and RCTs supports a role for optimising diet and targeted supplementation in the management of ADHD, particularly for subsets of individuals with specific dietary sensitivities or identified nutritional deficiencies. While these interventions are not a replacement for pharmacotherapy in most cases, they can serve as valuable adjuncts or, in select cases, alternatives. Clinical implementation should involve individualised assessment and multidisciplinary collaboration to ensure both safety and efficacy.
References
Abhishek, F. N. U., Gugnani, J. S., Kaur, H., & Damera, A. R. (2024). Dietary interventions and supplements for managing attention-deficit/hyperactivity disorder (ADHD): A systematic review of efficacy and recommendations. Cureus. https://www.cureus.com/articles/224893-dietary-interventions-and-supplements-for-managing-attention-deficithyperactivity-disorder-adhd-a-systematic-review-of-efficacy-and-recommendations.pdf
Bloch, M. H., & Qawasmi, A. (2011). Omega-3 fatty acid supplementation for the treatment of children with attention-deficit/hyperactivity disorder symptomatology: Systematic review and meta-analysis. Journal of the American Academy of Child & Adolescent Psychiatry, 50(10), 991–1000.
Chang, J. P., Su, K. P., Mondelli, V., Satyanarayanan, S. K., Yang, H. T., & Pariante, C. M. (2018). Omega-3 fatty acids in ADHD and related neurodevelopmental disorders: Meta-analysis of randomized controlled trials. World Journal of Biological Psychiatry, 19(2), 132–142.
Nigg, J. T., Lewis, K., Edinger, T., & Falk, M. (2012). Meta-analysis of attention-deficit/hyperactivity disorder or attention-deficit/hyperactivity disorder symptoms, restriction diet, and synthetic food color additives. Journal of the American Academy of Child & Adolescent Psychiatry, 51(1), 86–97.e8.
Pelsser, L. M., Frankena, K., Toorman, J., Savelkoul, H. F., Dubois, A. E., Pereira, R. R., ... & Buitelaar, J. K. (2017). Effects of a restricted elimination diet on the behaviour of children with attention-deficit hyperactivity disorder (INCA study): A randomised controlled trial. The Lancet, 377(9764), 494-503.
Shareghfarid, E., Sangsefidi, Z. S., & Djafarian, K. (2020). Empirically derived dietary patterns and food groups intake in relation with attention deficit/hyperactivity disorder (ADHD): A systematic review and meta-analysis. Clinical Nutrition ESPEN, 36, 1-9. https://www.sciencedirect.com/science/article/pii/S2405457719304863
Sonuga-Barke, E. J. S., Brandeis, D., Cortese, S., Daley, D., Ferrin, M., Holtmann, M., ... & Sergeant, J. (2013). Nonpharmacological interventions for ADHD: Systematic review and meta-analyses of randomized controlled trials of dietary and psychological treatments. American Journal of Psychiatry, 170(3), 275–289. https://psychiatryonline.org/doi/abs/10.1176/appi.ajp.2012.12070991
Wang, L. J., Wang, S. H., Huang, Y. S., & Su, L. Y. (2017). The efficacy of zinc supplementation for ADHD: A meta-analysis of randomized controlled trials. BMC Psychiatry, 17, 1-11.
Repairing the GUT wall
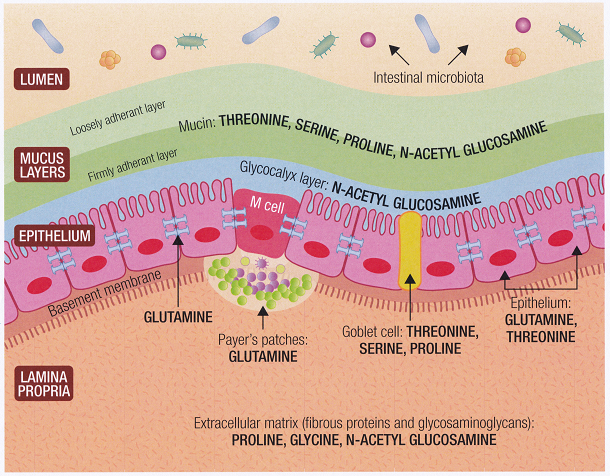
In addition to removing irritants from the diet, the gut wall needs to be repaired using specific nutrients, including Omega 3 EFAs and specific amino acids. The gut’s bacterial balance should be restored, through a reduction in sugar, refined carbohydrates, wheat, and cereal grains – all of which can be replaced with legumes and vegetables. Transitioning to this diet can take several months, but in our experience most children thrive on this diet, with parents and teachers reporting behavioural improvements. We see best results when children on this diet also take part in Neurotherapy, to address abnormal brainwave patterns, and CBT, to help them better adapt to their environment and promote functional behaviours.
Food allergies and abnormally high levels of naturally occurring bowel bacteria can increase amine production in the gut. Recent evidence suggests that these trace amines trigger the brain’s neurotransmitter receptors, resulting in mental fog, fatigue, and medication-resistant depression. This may be why ~ 40% or people respond to anti-depressants and 30% to placebo.
Omega 3 supplements are an important component of nutritional supplementation at BNC as part of our ADHD therapies, Learning Difficulties, and other developmental disorders.
Amines, depression, and impaired mental function in ADHD
Amines are naturally occurring substances in food, which the body can tolerate in small amounts. However, in larger quantities they can cause serious brain disturbances, triggering depression and reducing mental alertness. Recent studies examining amine receptors in the brains of mammals, including humans, suggest that increased dietary amines along with increased amine production from the overgrowth of certain gut bacteria, causes depression and a ‘scrambling’ of brain messages, resulting in a foggy mind and poor concentration.



