Symptoms of Post-Concussion Syndrome
What is Post-Concussion Syndrome
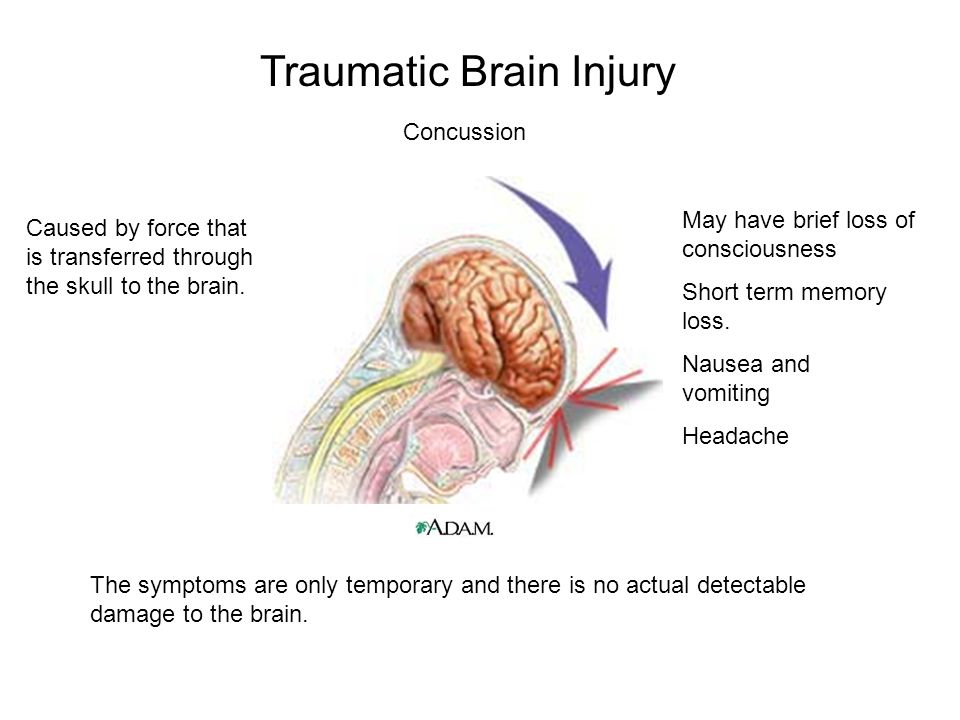
After a forceful blow to the head, the brain can move differently from the skull, leading to traumatic brain injuries (TBI). While much of the initial damage occurs at the point of impact, the brain’s frontal and temporal lobes are particularly susceptible to bruising—contusions—because of the way shock waves and shearing forces affect this delicate tissue. In some cases, a pressure wave travels through the brain and causes a “contrecoup” injury, resulting in additional contusions on the side opposite the initial impact. These forces can also shear axons at the junction of white and gray matter, further damaging neural connections (NIH Bookshelf; NIH Bookshelf on contrecoup injury).
The terms Post-Concussion Syndrome (PCS) or Post-Concussive Disorder refer to a collection of lingering symptoms that can persist long after a mild head injury. Although such injuries are typically considered minor, a significant number of people continue to experience symptoms for weeks, months, or even years after the event. These symptoms often include headaches, memory issues, difficulty socialising, and personality changes, and can overlap with conditions like Attention Deficit Disorder, Adjustment Disorder, and Mood Disorders (NIH Bookshelf; PMC). Notably, conventional MRI and CT scans often fail to reveal clear abnormalities in people suffering from PCS, despite the presence of these functional deficits (NIH Bookshelf; PubMed). This cluster of residual symptoms is referred to as ‘Post-Concussion Syndrome’.
Symptoms of Post-Concussion Syndrome
This clinic's psychologists provide support for the cognitive and psychological aspects of PCS. Physical symptoms such as headaches and dizziness should be assessed and managed by your treating medical practitioner.
- Attention deficits and difficulty sustaining mental effort are commonly seen in individuals with post-concussion syndrome (Mayo Clinic).
- Fatigue and tiredness frequently affect people after a concussion (NCBI Bookshelf).
- Impulsivity can emerge following a traumatic brain injury, sometimes leading to risky or inappropriate actions (ScienceDirect).
- Irritability and a low frustration threshold are often reported, sometimes resulting in outbursts or difficulty managing emotions (Headway).
- Temper outbursts have been observed as a behavioural effect of brain injury (Headway).
- Changes in mood, including depression and anxiety, are also common after a concussion (Cognitive FX).
- Learning and memory problems, such as trouble with concentration and memory, are typical symptoms (Mayo Clinic).
- Impaired planning and problem-solving abilities can arise after a concussion (ScienceDirect).
- Inflexibility and ‘concrete’ (rather than ‘fluid’) thinking may be present, making it harder to adapt to new situations (Headway).
- A lack of initiative is sometimes observed, with individuals appearing less motivated or proactive (ScienceDirect).
- Dissociation between thoughts and actions has been noted, where individuals may struggle to act on their intentions (NCBI Bookshelf).
- Communication difficulties, such as trouble expressing oneself or following conversations, are not uncommon (MSKTC).
- Socially inappropriate behaviours, including excessive disinhibition or not following social norms, are well-documented after brain injury (Cognitive FX).
- Self-centredness and a lack of insight, where individuals may not recognise their own issues or how their behaviour affects others, are frequently described (Headway).
- Poor self-awareness is a clinical concern, affecting outcomes and rehabilitation (PMC).
- Impaired balance, dizziness, and headaches are physical symptoms commonly reported in post-concussion syndrome (Physio-Pedia).
- Personality changes, such as shifts in emotional responses or overall demeanour, may persist after a concussion (Health.mil).
Although many people experience persistent symptoms after a brain injury, conventional scans like CTs or MRIs often fail to reveal any abnormalities. This diagnostic gap can lead to unfair stereotypes—individuals are sometimes labelled as “hot headed” or accused of having a “short fuse,” when these behaviours may actually stem from subtle, undetected brain changes (Neuropsychological Assessment, Lezak et al., 2012). These misunderstandings can result in misdiagnoses, such as mood or personality disorders, rather than recognising the neurological basis for the symptoms (Silver et al., 2009). Research shows that standard neuroimaging is often not sensitive enough to detect the microstructural or functional changes that underlie these issues (Bigler, 2013). More recently, advances in imaging have begun to reveal abnormalities in cases where traditional scans appear normal, underscoring the need for more sensitive diagnostic tools to accurately identify and address these injuries (Hillary et al., 2021).
Symptoms have an Organic Basis
There’s been a lot of debate around Post-Concussion Syndrome (PCS), especially since patients often report persistent symptoms even when standard scans show little or no injury. The question of whether PCS is psychological or rooted in actual brain changes has been the subject of ongoing research. Over the past three decades, mounting evidence from neuroimaging studies has shown clear organic, brain-based changes in people with PCS. For example, research using cerebral blood flow (CBF) imaging has found abnormal perfusion patterns in both children and adults with persistent post-concussion symptoms, linking these changes to symptom severity and recovery outcomes (Journal of Neurotrauma, JAMA Neurology, Journal of Neurotrauma 2021).
Neuropsychological testing consistently finds cognitive deficits in attention, memory, and executive function that correlate with PCS, even in the absence of visible structural damage on MRI scans (Neurology India, Journal of the International Neuropsychological Society).
Updated on: 22/02/2026 by: Dr. Jacques Duff – BA Psych; Grad Dip Psych; PhD; MAPS; MECNS; MAAAPB; MISNR; FANSA
Reviewed on: 28/02/2026 by: Bernard Ferriere - Clinical Psychologist; BA; Grad Dip Applied Psychology; Dip Clinical Hypnosis.
