National clinical guidelines for ADHD
Treatment and therapy options for ADHD
According to the Australian clinical guidelines for ADHD, best-practice management involves a multimodal approach that addresses both core symptoms and associated psychosocial difficulties. Stimulant medication is recommended as a first-line intervention, given its strong evidence base for reducing ADHD core symptoms and improving functioning. Careful monitoring is necessary, especially in the context of anxiety, as stimulants may exacerbate these symptoms or impact sleep. The guidelines recommend that a multimodal approach is more effective than any single option.
The following image from the Australian evidence-based clinical practice guideline for attention deficit hyperactivity disorder, graphically explains the medical and non-medical recommendation.
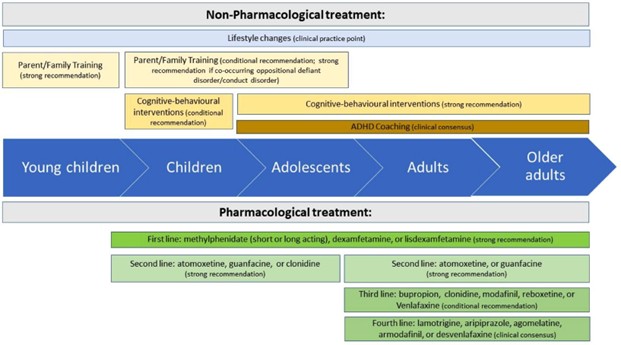
- Medication: Initiate a trial of stimulant or non-stimulant medication, titrated and monitored closely for efficacy and side effects, in line with national guidelines.
- Psychological Intervention: Cognitive behavioural therapy (CBT) to support emotional regulation, address comorbid anxiety and oppositional behaviours, and provide coping strategies for stress.
- Family Involvement: Engage parents in psychoeducation and ongoing support, promoting a collaborative approach to monitoring symptoms, implementing strategies at home, and managing stressors.
- Diet and Nutrition: Referral for a nutritional assessment if presentation suggest possible nutritional deficits (e.g., suboptimal energy, fatigue, focus issues). Dietary interventions should focus on balanced macronutrient and micronutrient intake, regular meals, and, if needed, supplementation under clinical recommendation and professional supervision.
- Lifestyle Modifications: Encourage regular physical activity, consistent sleep routines, structured daily schedules to optimise attention and mood stability and supportive school accommodations and environmental modifications.
Regular follow-up is essential to review symptom progression, treatment response, and emerging needs.
Reviewed on: 28/02/2026 by: Bernard Ferriere - Clinical Psychologist; BA; Grad Dip Applied Psychology; Dip Clinical Hypnosis.
MAPS: Member, Australian Psychological Society
MASH: Member, Australian Society of Hypnosis
FCCP: Fellow of the College of Counselling Psychologists (UK)



