PANS/PANDAS Syndrome
Symptoms of PANS or PANDAS
The information provided on this page is for psychoeducation only. PANS and PANDAS require medical diagnoses. Our practitioners do not diagnose or treat PANS or PANDAS. Our psychologists can offer psychological support, psychoeducation , and a nutritionist or dietician may provide nutritional support to potentially repair brain cells damaged by the autoimmune system. We can however to medical practitioners who can diagnose and treat those disorders.
Historical perspective of PANS and PANDAS
In 1990, researchers at the National Institutes of Health (NIH) observed that a subset of children experienced a sudden onset of tics and/or obsessive-compulsive disorder (OCD) following bacterial or viral infections. They initially labelled this condition "Paediatric Infection-Triggered Autoimmune Neuropsychiatric Disorders" (PITANDS), reflecting the idea that various infections—not just streptococcal—could trigger abrupt neuropsychiatric symptoms such as tics or OCD in children Tourette Syndrome, TK Murphy.
Soon after, further research at the NIH, particularly by Dr. Susan Swedo and colleagues, identified that many of these cases followed infections with group A beta-haemolytic streptococci (GABHS). To describe this more specific phenomenon, they coined the term "Paediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections" (PANDAS). The diagnostic criteria for PANDAS focused on the acute onset of symptoms, association with streptococcal infection, and the presence of neuropsychiatric symptoms like tics or OCD Paediatrics & Child Health, C Wilbur et al. PANDAS Network.
As research progressed, it became evident that similar acute-onset neuropsychiatric symptoms could also be triggered by infections other than streptococcus or sometimes even without a clear infectious trigger. This led to the development of a broader diagnostic category called "Paediatric Acute-onset Neuropsychiatric Syndrome" (PANS). PANS encompasses cases with sudden-onset OCD and/or severely restricted food intake, along with other neuropsychiatric symptoms, regardless of the infectious agent involved Journal of Child and Adolescent Psychopharmacology Paediatrics & Child Health. This evolution reflects both clinical observation and the ongoing effort to understand the complex relationship between infections, immunity, and neuropsychiatric symptoms in children.
PANDAS is a medical diagnosis
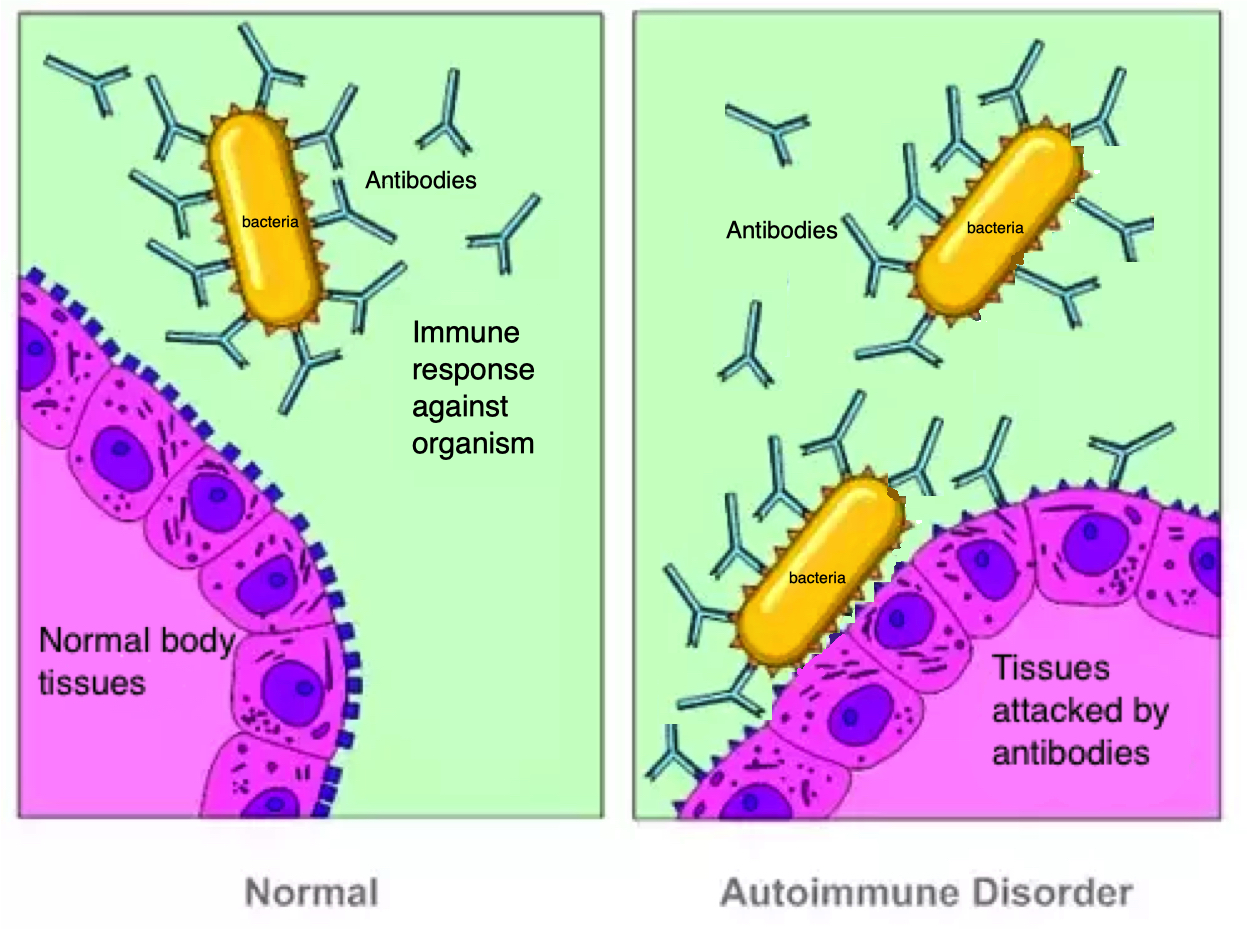
PANDAS is a medical diagnosis for children who develop sudden onset of neuropsychiatric symptoms, such as tics or obsessive-compulsive behaviours, following an infection with Group A beta-haemolytic Streptococcus (GABHS), the bacteria behind strep throat and scarlet fever. In certain genetically predisposed children, the immune system’s response to the infection can mistakenly target the brain’s basal ganglia due to a mechanism called “molecular mimicry.” This leads to neuropsychiatric symptoms similar to those seen in Sydenham chorea, another post-streptococcal neurological disease. Symptoms can include tics, abrupt OCD behaviours, anxiety, behavioural regression, handwriting changes, and cognitive inflexibility (Europe PMC; Taylor & Francis; MDPI - 2024).
PANDAS is also a MEDICAL Diagnosis

PANS is a broader diagnosis that includes all sudden-onset cases of obsessive compulsive disorder (OCD) or restricted eating—regardless of the specific infectious or non-infectious trigger. PANS requires the acute onset of severe OCD or eating restrictions, along with at least two additional cognitive, behavioural, or mood symptoms, such as irritability, anxiety, or depression (depositolegale.it).
Treatment for PANDAS and PANS
For PANDAS, antibiotics can help treat the underlying infection, but the symptoms are due to immune activity against the brain, not the bacteria itself. Therefore, antibiotics may not immediately resolve neuropsychiatric symptoms.
Behavioural interventions, psychological therapy, and supportive care are the mainstays of management. There is debate about long-term antibiotics; decisions should be individualised. Some evidence supports nutritional support for brain health, but strong clinical trials are lacking (MDPI - 2022).
Updated on: 20/02/2026 By: Dr. Jacques Duff – BA Psych; Grad Dip Psych; PhD; MAPS; MECNS; MAAAPB; MISNR; FANSA
Reviewed on: 20/02/2026 by: Bernard Ferriere - BA; Grad Dip App Psych; Dip Clinical Hypnosis; FCCP; MAPS; MASH; Clinical Psychologist
